
The intelligence layer for healthcare reimbursement strategy.
ReimburseIQ transforms federally mandated payer pricing data into automated negotiation intelligence for independent healthcare providers — turning reimbursement opacity into targets, leverage signals, and measurable revenue lift.
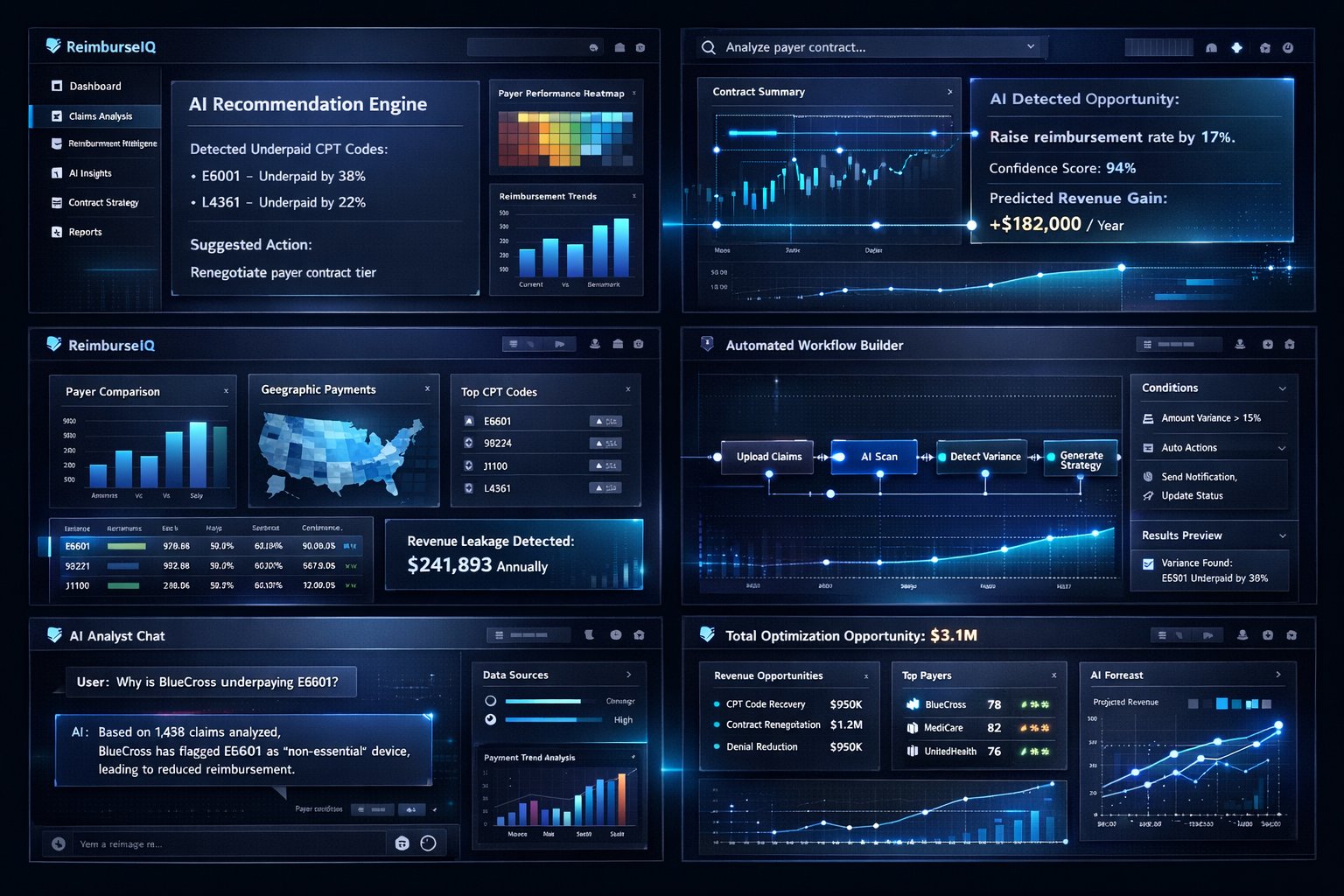
Built on a federally mandated data infrastructure.
Where the data comes from
ReimburseIQ's benchmark layer is built on rates reported directly by health insurance companies under federal price transparency mandates — the No Surprises Act and CMS machine-readable file requirements. These are rates insurers are legally required to publish, giving us a legitimate, expanding, regulatory-backed data source that improves in coverage over time.
Current coverage includes large national PPO plans. HMO plans and a growing set of regional payers are coming soon. Data refreshes quarterly to ensure current market signals.
Why this is defensible
The raw machine-readable files are notoriously large, inconsistently formatted, and difficult to parse at scale. Our proprietary peer-reviewed methodology for transforming that raw data into clean, actionable benchmarks is the moat — not just access to the underlying source.
Each new customer strengthens the benchmark accuracy of the intelligence layer, improving recommendations and tightening spread analysis over time. The data advantage compounds with scale.
Land small. Expand fast.
Entry product drives proof-of-value quickly. Core SaaS converts on clear ROI. Enterprise and licensing become the long-term infrastructure play.
- Benchmark + payer spread summary
- Negotiation readiness signal
- ROI estimate + recommended next steps
- Drives PRO subscription conversion
- CPT benchmarks — billing code comparisons
- Regional deltas — what peers are paid locally
- Payer spread analysis — insurer-to-insurer variance
- Monitoring + alerts for contract changes
- Multi-site dashboards + rollups
- Operator reporting automation
- Expanded benchmarking cohort controls
- Org-level monitoring + permissions
API integrations, custom data pipelines, advanced segmentation. For PE-backed clinic networks, RCM vendors, and device manufacturers.
The long-term infrastructure play: ReimburseIQ as a reimbursement data layer for analytics platforms, RCM vendors, and healthcare AI systems.
Conservative to platform-scale outcomes.
Projections assume blended ARPA across PRO/TEAM tiers, 15% Clarity Report to PRO conversion, and 45-day average sales cycle at lower tiers. Enterprise revenue begins Year 2–3.

~1,200 customers, primarily PRO conversions
~6,000 customers, high funnel volume + inside sales
Enterprise networks + licensing as infrastructure layer
Automated acquisition → inside sales scale
Phase 1 — Validate (0–90 days)
Clarity Report funnel + conversion playbook. Repeatable onboarding templates. Tight vertical focus on independent clinics.
Phase 2 — Inside Sales Engine (6–18 months)
SDR team + dialed outbound sequences. Clinic list-building at scale. Demo-to-close system + fast activation.
Phase 3 — Partner Distribution (18–36 months)
RCM / billing partners + co-sell distribution. Group and network rollups. API + licensing revenue streams.
The market conditions are urgent.
Payer complexity is rising
Reimbursement rates grow more fragmented every year. Independent practices are increasingly outgunned in negotiations without modern intelligence tools.
Price transparency creates urgency
Federal transparency mandates are making payer data more available — creating both the data source and the awareness that better information is possible.
Consolidation pressure is real
Independent practices face acquisition pressure from large health systems. Protecting margins through reimbursement intelligence is an existential need, not a nice-to-have.
ReimburseIQ is raising $650K.
SAFE Note
$5M Pre-Money
18 Months
Sales · Product · Data
Full use-of-funds breakdown, 18-month milestones, and investor deck available on request. Response within 24 hours.
